A Quality Focus
High Reliability in Action:
Improving Systems, Reducing Errors, Preventing Harm
NMC continues forward with our emphasis on being a “High Reliability Organization” (HRO) as support of our mission to provide exceptional care for our community. Embracing High Reliability means using intentional, proven tools and approaches to maintain exceptional care and service within a highly complex, high risk environment where any error could result in avoidable harm.
“It’s not that we will never make mistakes,” says Dr. John Minadeo, NMC’s Chief Medical Quality Officer, “It’s that we take the right steps to prevent mistakes and to not let mistakes cause harm.”
Through team education and engagement in High Reliability and the use of Lead Daily Management techniques, NMC has made significant progress in safety and quality improvements. This work produces immediate benefit to patients and staff – and is reflected in our advancement toward our ultimate goals of providing CMS 5-Star level care and Leapfrog A rated level care.
Here are two quick examples of improvement efforts from Fiscal Year 2023.

Respiratory Therapy:
Respiratory Therapy (RT) utilized their Key Process Indicator (KPI) board to track their device set up process throughout the hospital. (A KPI board is a data-driven tool facilitating staff-directed process
improvement with visible results – NMC leaders round on 19 active KPI boards throughout the organization each day.)
After collecting data that demonstrated an inconsistent process for how the respiratory medical devices are set up between use, the RT team performed a 5-why. (A 5-why is a formal Lean tool which helps a group go beyond surface appearances and find what is truly impacting a situation.) Their 5-why led to an action plan of developing a checklist of cleaning, setup, and equipment needed for each device. Since developing this checklist, they reduced their occurrences of missed setups or equipment by 77%.
From what they learned in that effort, the RT team then focused their effort on one specific device and has met their goal 95% of the time. Not only have they been able to create a process that increases patient safety, but they have also identified opportunities that they are looking to measure next. Ensuring RT has what they need when they need it is a vital component of patient safety.

Patient Access:
Patient Access has been diligently tracking patient identification errors at the time of registration or scheduling on their KPI board. Any error in patient identification carries the risk of the wrong care being provided to a patient, which could have serious consequences.
With a team-focus on finding system improvements to reduce errors to prevent harm (rather than an outdated and improvement inhibiting blame seeking focus), the Patient Access team carefully tracked their performance. When trends were discovered on their Pareto Chart (a statistical tool that helps turn raw data into actionable insight), the team worked on a 5-why to create an action plan. This action plan resulted in an 83% reduction in errors by the following month. As they monitored their work and noticed further data trends, another 5-why and action plan were performed, creating another decrease in errors. This work toward High Reliability has eliminated rework, prevented harm, and made for a much safer care environment.
New Web Presence Gives Public A Look at NMC Quality and Safety
As a way to share information about our care quality with the community, NMC published a new series of webpages on our site that highlight the ongoing work toward the delivery of safe, high-quality care.
The pages focus on three key quality initiatives from our Quality Plan and established best practices for hospitals: Hand Hygiene, Sepsis and Hospital Acquired Infections.
The pages offer information on what kind of data we are measuring, how NMC is performing in achieving our goals, what improvement projects are in work, and how patients and visitors can help.
Processes That Drive Result

Sepsis: NMC’s intentional focus on early identification and treatment
When bacteria get into a person’s body, it can cause an infection such as a urinary tract infection or pneumonia. If left untreated, these infections can cause sepsis. Sepsis is the body’s extreme response to infection and triggers a chain reaction throughout your body. Without timely treatment, sepsis can rapidly lead to tissue damage, organ failure, and death.
As outlined in NMC’s Quality Plan, the hospital is working to ensure we deliver time-sensitive care for patients with sepsis that meets standards set by the Centers for Medicare and Medicaid.
Progress this year included:
- Staff education
- Improved workflows between departments like the Emergency Department and our inpatient unit
- Order sets for providers to use, ensuring consistency with treatment protocols for sepsis patients
- Screening during triage for all adult patients in the Emergency Department
- Screening for admitted patients at least every 12 hours
These screenings are part of a new standardized surveillance process that includes:
- Specific required questions to be asked of all adult ED patients during triage
- Documentation in the medical record required from inpatient nursing staff every 12 hours
- Based on the response and certain vital signs meeting sepsis criteria, the medical record system will assist the nurse in identifying possible sepsis patients and provide a sepsis risk assessment.
- If the patient doesn’t meet all criteria at the time of screening, but does have the potential for sepsis, the system will surveil during the visit and flag nursing/providers if the patient should meet criteria at a later time.
- If a patient screens positive, the system displays a “flag” on the tracker board to alert the care team.
- Care providers are able to easily locate criteria triggering the sepsis alert for patients identifying as septic.
- Nurses can implement sepsis orders in the ED more confidently.
The goal of this work is to identify and treat sepsis early and effectively. As NMC progresses, we will measure our success by tracking rates of compliant care, aiming to be well above the national average.
Preventing Readmissions
Ensuring that patients are able to go home from the hospital and recover well from their illness or injury is a key factor in the exceptional care that NMC strives to provide. NMC is committed to helping patients and caregivers to that patients do not need to be unnecessarily readmitted.
NMC’s Quality Plan outlines a goal for the hospital to keep the readmission rate below nine percent, and the Utilization Review Committee meets regularly to review data and processes and seeks to find ways to improve.
“We want to transition our patients out of the hospital safely, and we want to deliver holistic clinical care,” says Manager of Care Management Amanda Wilson. “We want to take care of your whole human body and make sure that you don’t need to come back to us.”
The Utilization Review Committee monitors readmissions related to specific conditions like Congestive Heart Failure (CHF), Chronic Obstructive Pulmonary Disease (COPD), respiratory failure, pneumonia and others.
NMC has seen an improvement in readmission rates for CHF, which are down to 17.46 percent for fiscal year 2023.
Strata internal claims-based data
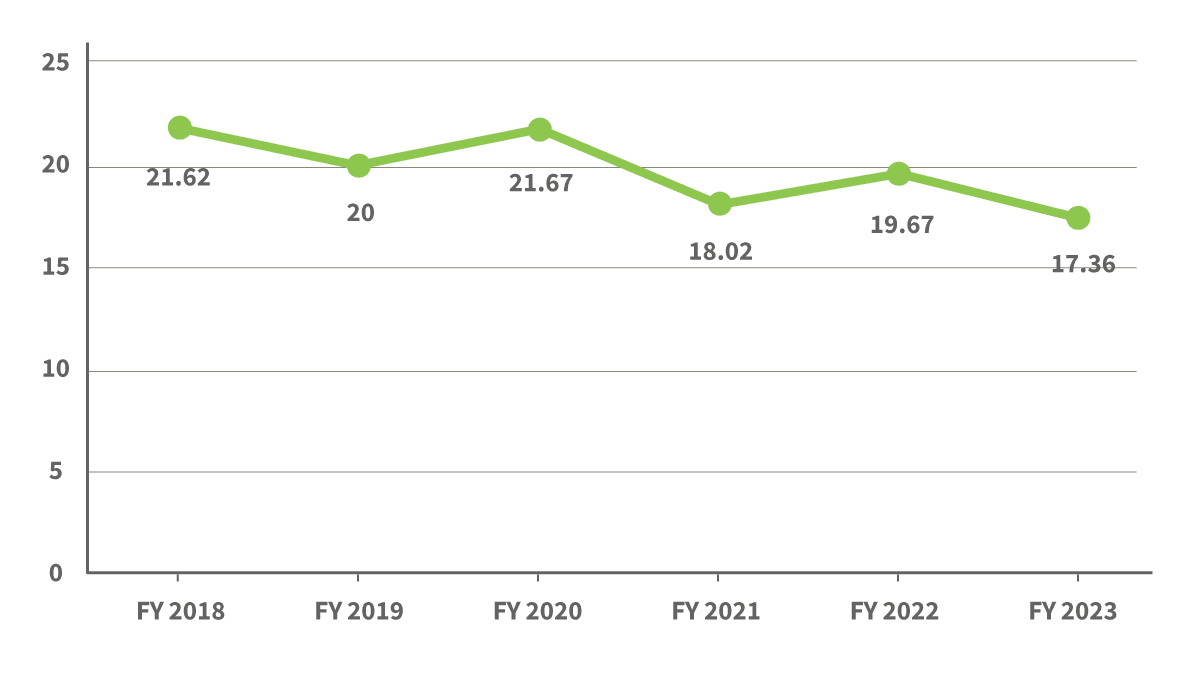
With an intentional focus on supporting patients with Congestive Heart Failure this year, we are seeing good progress.
Premier risk-adjusted data
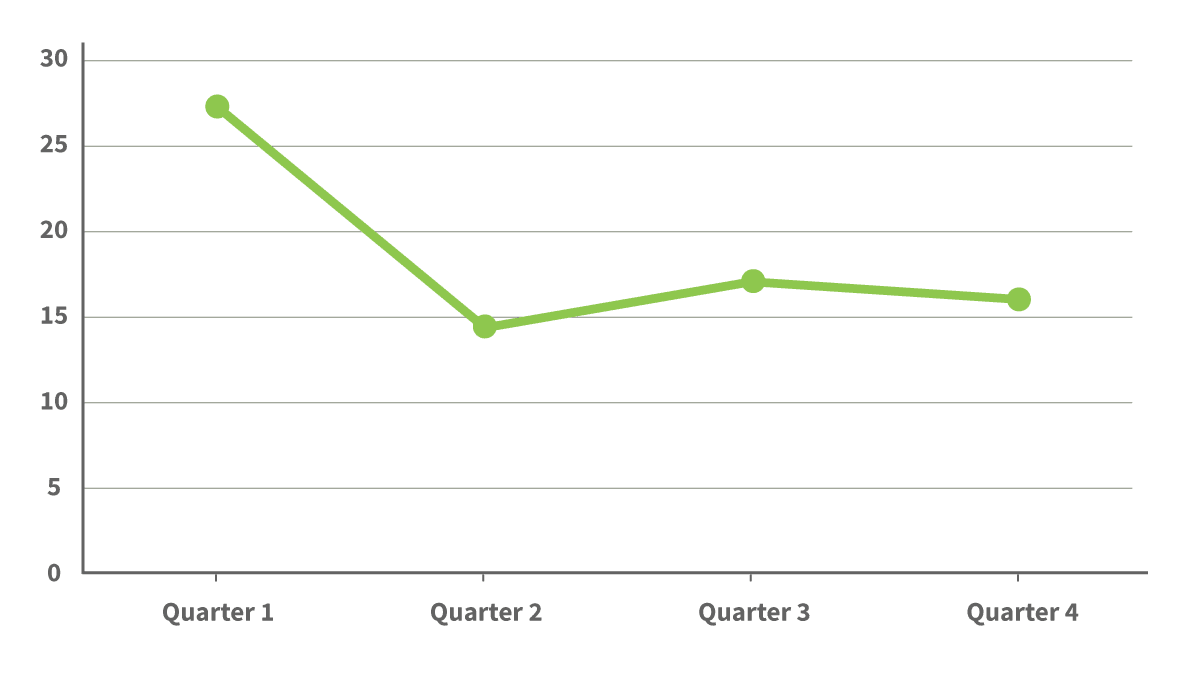
To achieve these improvements, a workgroup on readmissions has developed strategies to tackle the complex issue, including:
- Implementing a collaborative discharge checklist that ensures all members of the care team prepare the patient and their care partner to go home.
- Communication with a care partner for every patient
- Use of the LACE tool which helps predicts and prevent high-risk conditions that could result in readmission
- Creation of a workgroup with skilled nursing facilities to ensure seamless transitions from the hospital to those settings
- Use of Key Performance Indicators to monitor readmissions on a daily basis
- Utilizing surveillance of all patients with COPD or CHF to ensure equity of care and support.
- Invigorating a workgroup on palliative care, implementing an automatic trigger in certain circumstances so that patients and families get palliative consultation.
“It’s been a very collaborative effort,” says Wilson. “We are partnering with home health agencies, skilled nursing facilities, primary care practices and many more to support the health and wellbeing of our community.”
CAIRES Circle ACH
Our community formed a new Accountable Community for Health (ACH) organization this year called C.A.I.R.E.S. CAIRES Accountable Community for Health (ACH) brings together partners from health care, social services, and other sectors, as well as representation from the community, to take responsibility for the health of Grand Isle and Franklin counties.
Addressing health inequities in our region’s service delivery system is the driving force in the design of this new Accountable Community for Health. CAIRES is committed to staying grounded in health equity by ensuring all work is designed with health equity principles.
The CAIRES circle is a team that meets monthly and is focused on the sustainability of the ACH. Work groups form on topics or issue areas to coordinate work around shared goals and strategies. An example would be a work group that formed in the summer of 2023 to focus work on the needs of children in Franklin and Grand Isle Counties.
CAIRES Guiding Principles:
- Collaboration
- Adaptability
- Inclusiveness
- Respect
- Equity
- Sustainability
CAIRES Member Organizations:
- Abenaki Nation of Missisquoi
- Agency of Human Services – St. Albans and Middlebury Districts
- AgeWell
- Bayada
- Bi-State
- Bridges to Health, UVM
- CarePartners
- Cathedral Square
- Champlain Valley Head Start
- CIDER
- Cold Hollow Family Practice
- Franklin County Caring Communities
- Franklin County Industrial Development Corporation
- Franklin Grand Isle Community Action - CVOEO
- Franklin Northeast Supervisory Union
- Franklin West Supervisory Union
- Grand Isle Sherriff’s Office
- Grand Isle Supervisory Union
- Howard Center
- Maple Run Unified Supervisory Union
- Missisquoi Valley School District
- Monarch Maples Pediatrics Enosburg
- Northwest Regional Planning Commission
- Northwestern Counseling and Support Services
- Northwestern Medical Center
- NOTCH
- OneCare Vermont
- Planned Parenthood of Northern New England
- Primary Care Health Partners – St. Albans Primary Care
- St. Albans Primary Care
- Samaritan House
- Sheldon Food Shelf
- Spectrum
- St. Albans Museum
- St. Albans Police
- Suncrest Health Care Communities
- United Way of Northwest Vermont
- Vermont Department of Health Division of Substance Use
- Vermont Department of Health St. Albans Office of Local Health
- Vermont Dept of Children and Families, Family Services Division
- Voices Against Violence
- VTNG

NMC Earns Gold Seal of Approval
In 2023, Northwestern Medical Center once again earned The Joint Commission’s Gold Seal of Approval® for Hospital Accreditation by demonstrating continuous compliance with its performance standards. The Gold Seal is a symbol of quality that reflects a health care organization’s commitment to providing safe and quality patient care.
NMC underwent a rigorous, unannounced onsite review on December 10, 2022. During the visit, a team of Joint Commission reviewers evaluated compliance with standards spanning several areas including emergency management, environment of care, infection prevention and control, leadership, and medication management.
The Joint Commission’s standards are developed in consultation with health care experts and providers, measurement experts and patients. They are informed by scientific literature and expert consensus to help health care organizations measure, assess, and improve performance. The surveyors also conducted onsite observations and interviews.
